About ANCA-Associated Vasculitis (AAV)
- 3 types:
- Granulomatosis with polyangiitis (GPA)
- Microscopic polyangiitis (MPA)
- Eosinophilic granulomatosis with polyangiitis (eGPA)
- Insidious onset, weeks-months
- eGPA mean age ~40
- Associated with atopy (asthma, eczema, sinusitis)
Disease Overview & Clinical Presentation
- Adult with new-onset asthma: consider eosinophilic granulomatosis with polyangiitis (eGPA)
- Granulomatosis with polyangiitis on DDx (view image) for:
- New diagnosis of otitis media as adult
- Recurrent sinusitis +/- epistaxis
- Pseudotumor
- Nasal septal perforation
- Pulmonary renal syndrome
- Often with:
- Constitutional symptoms
- High CRP
- ESR can be >100
- cANCA+ PR3: consider GPA
pANCA+ MPO: consider MPA - Look for potential medications for drug-induced vasculitis
- ANCA neg does not rule out AAV
- ANCA usually neg in cardiac-associated eGPA or upper airway limited GPA
Treatment
- Need PJP prophylaxis for AAV lung disease and treatment with rituximab or cyclophosphamide
Common Symptoms
- Constitutional symptoms
- Episcleritis/scleritis
Granulomatosis with Polyangiitis (GPA)
- Pulm-renal
- Cavitary pulm lesions
- Upper airway limited (ANCA neg)
- Pseudotumor
- Nasal septal perforation
Microscopic Polyangiitis (MPA)
- Pulm-renal (ANCA pos when renal dz)
Eosinophilic Granulomatosis with Polyangiitis (eGPA)
- Cardiac involved (ANCA neg):
- Pericardial effusion
- Myocarditis
- Mononeuritis multiplex (foot drop)
Lab Workup
- ANCA panel
- cANCA+PR3=GPA
- pANCA+MPO=MPA
- pANCA/MPO in EGPA ~50%
- HH CRP, HH ESR
- Anemia
- AKI
- Urinalysis:
- +blood
- +protein
- +RBC casts
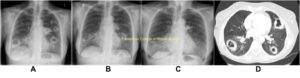
Imaging
- CT chest (view images)
- Diffuse infiltrates in DAH
- Cavitating lung lesions in GPA
Bronchoscopy
- Confirm DAH
Kidney Biopsy
- Pauci-immune crescentic glomerulonephritis (GN)
Drug Induced
- PTU, hydralazine, minocycline
- Goodpasture (GBM disease)
Malignancy
- Lymphoma
- Leukemia
Other Kidney Disease
- Lupus nephritis
- Membranous nephropathy
- IgA nephropathy
- Post-infectious glomerulonephritis (GN)
- Usually with rheumatology supervision
- Two-part approach: induction and maintenance
Induction
- Pulse steroids (500-1000 mg IV for 3-5 days) PLUS
- Follow with prednisone taper
Maintenance Choices
Monitoring
- PJP prophylaxis needed for pts with lung disease and treatment with rituximab or cyclophosphamide
- Monitor:
- Renal function
- Urinalysis
- For infection from immunosuppression
Prognosis
- 90% mortality risk if untreated
- GPA more likely to relapse
- MPA more like to progress to interstitial lung disease (ILD)