About Spondyloarthritis
Spondyloarthritis is a group of related disorders, including:
- Psoriatic arthritis
- Ankylosing spondylitis
- IBD-associated arthritis
- Reactive arthritis
Typically negative for RA antibodies (RF, CCP)
Disease Overview & Clinical Presentation
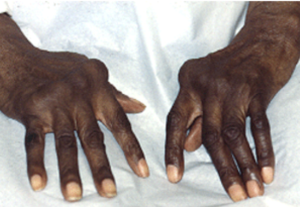
- Inflammatory arthritis of DIPs – PsA high on DDx
- Inflammatory back pain of young – start with SI joint radiographs
- Classic triad of reactive arthritis = conjunctivitis, urethritis, and arthritis (most patients do NOT have all three features)
Diagnostic Workup & Differential Diagnosis
- High suspicion for sacroiliitis but negative XR consider STIR MRI of pelvis
- HLA-B27 positive has high population prevalence. HLA-B27+ doesn’t equate to spondyloarthritis diagnosis.
- If suspicious for psoriatic arthritis but don’t see obvious psoriasis – examine ears, scalp, umbilicus, gluteal cleft
- Spinal fusion in ankylosing spondylitis associated with increased risk of spinal fracture
Treatment
- NSAIDs first line for spondyloarthritis
Typical Manifestations
- “Inflammatory back pain”
- Age < 40
- Better with exercise
- Worse with immobility
- Nocturnal symptoms
- Alternating buttock pain
- Other arthritis
- Predilection for knees, ankles
- Enthesitis
- Dactylitis (“sausage digit”)
- Uveitis
Association with Derm and GI diseases
- Psoriatic arthritis (look for nail pitting)
- Gut disease:
- Crohn’s disease
- Ulcerative colitis
- Celiac disease
- Infection (Reactive)
- Usually GU/GI infection
Lab workup
- CBC, CMP, ESR, CRP
- HLA-B27
Synovial fluid
- Inflammatory (2K-50K WBC/microL)
Imaging
- Sacroiliac joints
- XRay
- MRI with STIR: sclerosis, erosions, “pseudo-widening”,
fusion if advanced
- Peripheral joints
- Can show “pencil-in-cup” deformity for hand
- Hand Psoriatic arthritis associated with nail disease
- +/- Extra bone formation at entheses: nonspecific
Other rheumatic
- Rheumatoid arthritis
- Lupus
- Crystalline arthritis (gout, CPPD)
Infectious
- Gonococcal arthritis
- Infectious sacroilitis (typically unilateral)
Non-inflammatory
- Osteoarthritis
- Mechanical back pain/degenerative disease
- Fibromyalgia
- DISH
Peripheral Arthritis
- NSAIDs
- Conventional DMARDs: sulfasalazine, methotrexate
- Biologics (inhibitors of TNF, IL-17, IL-23, IL-12/23)
- JAK inhibitors
- Apremilast
Axial Arthritis
- NSAIDs first line
- TNF inhibitors
- IL-17 inhibitors
- JAK inhibitors
General Measures
- Treat infection
- Physical therapy
- Coordinate with derm or GI as necessary
Monitoring
- Monitoring for complications of therapy
- Reactive arthritis
- Many cases resolve (months), but minority develop chronic arthritis requiring ongoing treatment
Complications/Associations
- Inflammatory eye disease – uveitis, conjunctivitis
- Ankylosing spondylitis
- Aortic regurgitation
- Aortitis
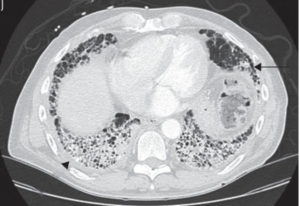
- Apical pulmonary disease