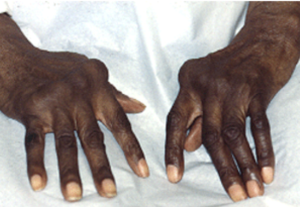
About Juvenile Idiopathic Arthritis (JIA)
JIA is an inflammatory autoimmune disease that primary impacts the joints.
- Prevalence: 7-401/100,000 children
- Interplay of environment and genetics
Clinical Presentation
- Silent uveitis can cause permanent eye damage
-
- More likely in ANA positive, younger patients with newer disease
- Need a slit lamp exam to screen for this
- TMJ can be a silently involved joint with significant damage ramifications
Treatment
- Treat to target with early aggressive therapy to prevent joint damage
- Methotrexate is first line gold standard DMARD
- Insidious, chronic arthritis > 6 weeks duration
- Can be symmetric or asymmetric, oligoarticular or polyarticular
- Oligoarticular
- < 4 joints
- Most common subtype
- Large joints more common
- Asymptomatic uveitis
- Polyarticular
- RF
- >4 joints
- Symmetric
- Large and small joints
- RF+
- Early onset RA
- RF
- Oligoarticular
- >1hr AM stiffness that improves with activity
- Extra-articular manifestations:
- Uveitis
- Inflammatory bowel disease
- Psoriasis
- Dactylitis
- Nail pitting/onycholysis
- Psoriasis in family
- Asymmetric, large and small joints
Lab workup
- Inflammatory markers (ESR, CRP)
- CBC for anemia of chronic disease
- CMP
- ANA
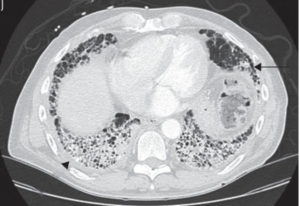
Imaging
- X-rays are less helpful
Other Rheum Disease
- SLE
- Sjogren’s
- Sarcoid
More Acute
- Viral arthritis
- Toxic synovitis
Treat to target
Acute Treatment
- NSAIDs (don’t modify disease)
- Steroids (modify disease but high side effect profile)
Chronic Treatment
- DMARDs (methotrexate, leflunomide)
- Biologics (TNF inhibitors, IL-6 inhibitors, others)
- Disease activity measurements (e.g. CJADAS)
- Early treatment of inflammation to prevent joint damage