About Systemic Lupus Erythematosus (SLE)
System lupus erythematosus (SLE) is a chronic multisystemic autoimmune disease.
- Autoantibodies deposit within tissues and fix complement
- Multifactorial etiology: Interplay between genetic, environmental, and hormonal factors
- Predominantly affects young women in childbearing years
- Peak age of onset: 15 – 45 y.o.
- Racial and gender disparities exist in terms of organ involvement, disease severity and response to therapy
- Reported worldwide prevalence frequencies range from 20 to 240 per 100,000 people
- Reported worldwide incidence rates range from 1 to 10 per 100,000 person-years
Disease Overview & Diagnostic Workup
- Lupus is a complex multisystemic disease.
- Diagnosis is made clinically based on symptoms and signs.
- Use laboratory data to confirm the diagnosis.
- ANA is a hallmark of lupus but it is not specific for lupus.
- Sun exposure can precipitate flares of lupus.
- Preventative health measures should be taken to prevent disease flares and complications.
Treatment
- Hydroxychloroquine is recommended for all patients with lupus.
- Choice of immunosuppressive therapies depends on organ involvement.
Heterogeneous disease
Cutaneous
- Alopecia
- Photosensitive rashes
- Discoid rash
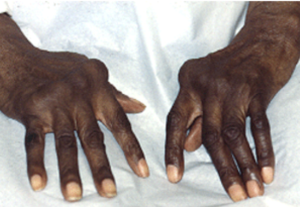
Musculoskeletal
- Arthralgias
- Jaccoud’s arthropathy
Ocular
- Periorbital swelling
- Retinal vasculitis
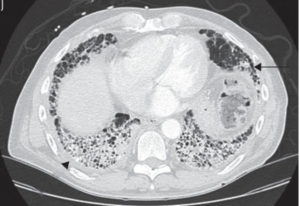
Serositis
- Pericarditis
- Pleuritis
Cardiovascular
- Libman-Sacks endocarditis
Renal
- Nephritis
Hematologic
- Leukopenia
- Anemia
- Thrombocytopenia
Neurologic
- Seizures
- Psychosis
- Cerebrovascular accidents
SLE is diagnosed clinically using a combination of clinical features and supporting labs.
Lab Workup
- Antinuclear antibodies (ANA)
- Laboratory hallmark of SLE
- >98% of SLE patients have a positive ANA. However, ANA is not specific for SLE (up to 33% of healthy adult population has a +ANA but only ~ 5% will develop SLE).
- Other antibodies: anti-dsDNA, anti-Smith, SSA (anti-Ro), SSB (anti-La), antiphospholipid antibodies
- CBC, CMP, urinalysis, UPC, complement levels
Imaging & Biopsy
- Imaging studies and renal biopsy might be required
Differential diagnosis is broad.
- Other connective tissue diseases
- Scleroderma
- Sjogren’s
- Mixed connective tissue disease
- Systemic vasculitis
- Sarcoidosis
- Lymphoma
- Infective endocarditis
- Viral infections (EBV, hepatitis C, HIV, etc.)
Sun Avoidance
- UV light exposure can exacerbate cutaneous rashes & cause flares)
- Patients should wear protective clothing & use sunscreen regularly
Pharmacotherapy
- Pharmacotherapy choice is based on organ involvement
- Hydroxychloroquine:
- Best long-term Rx
- Recommended for all patients with systemic lupus
- NSAIDs: Can be used for arthralgias
- Local or systemic glucocorticoids: for acute exacerbations
- Immunosuppressive agents (e.g., mycophenolate, azathioprine, cyclophosphamide, belimumab, etc.)
- For organ threatening manifestations such as glomerulonephritis
- Used a steroid-sparing agents
- Disease activity measures:
- SLEDAI
- BILAG
- Encourage regular clinical and lab monitoring by a rheumatologist
- Lupus is an independent risk factor for cardiovascular disease
- Emphasize smoking cessation
- Manage BP, lipids
- Screen for diabetes
- Encourage maintenance of healthy weight
- Slightly higher risk of overall cancer development due to lupus
- Emphasize need for malignancy screening
- Discuss reproductive health
- Assess bone health
- Risk of vitamin D deficiency due to sun avoidance and decreased bone density from glucocorticoid use and inflammation