A 75 yo F with Hx of DM2, HTN and OA presents with progressive stiffness originating in her shoulders and neck with more recent involvement of the bilateral lateral hips for 5 weeks.
History
- Symptoms present in the morning and improve with activity.
- Acetaminophen provides minimal relief.
Physical Exam
- Normal VS
- Pain with palpation of shoulders and lateral hips, preserved strength
- No evidence of swelling in small joints of hands and feet
- 5/5 strength in upper and lower extremities
Diagnostic Workup
- Labs: CRP 31 (H), ESR 75 (H), CBC with mild normocytic anemia, CMP wnl
- Imaging: Shoulder x-ray with mild degenerative changes bilaterally
Treatment
- Prednisone 20mg per day resolved patient’s symptoms within 48 hours but blood sugar uncontrolled
- Second line treatment: Patient started on SQ sarilumab with ability to taper off of steroids and without recurrence of PMR symptoms
An 80 yo M with hx of HLD, CAD presents with new onset of unilateral headaches refractory to OTC medications including NSAIDs and acetaminophen.
History
- No vision changes
- Few weeks of girdle stiffness
- Symptoms of tiredness when chewing on food for long, such as food like steak
Physical Exam
- Normal VS
- Shoulders tender to palpation bilaterally
- Scalp tender to palpation over the area of the temporal artery with diminished temporal artery pulse on right (view image)
- High dose steroids started for high suspicion of giant cell arteritis.
Diagnostic Workup
- Labs: CRP 50, ESR >120, CBC and CMP wnl
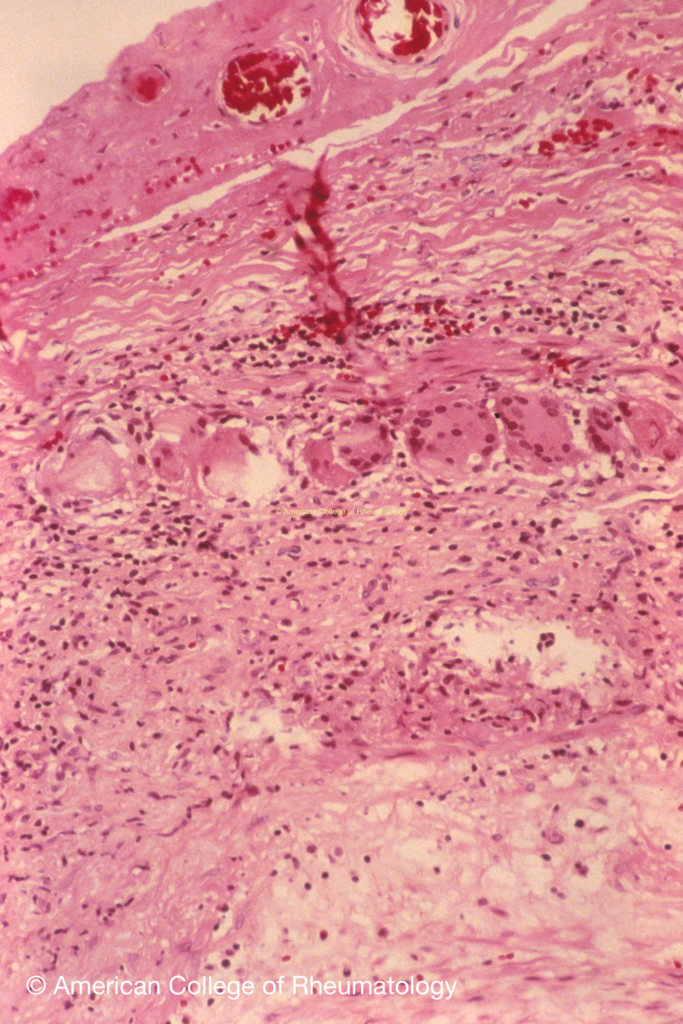
- Biopsy:
- Temporal artery biopsy pathology obtained within 2 weeks of steroid start.
- Granulomatous inflammation of the inner half of the media, centered on the internal elastic lamina, with a mononuclear infiltrate, multinucleated giant cells, and fragmentation of the internal elastic lamina (view image)
Treatment
- High doses of systemic steroids with improvement in headache
- Also started tocilizumab to decrease steroid burden, given patient’s CAD