About Sarcoidosis
Sarcoidosis is an autoimmune disease with increased inflammation and organ infiltration driven by granuloma formation.
-
Females = males
- Average age of diagnosis: 40-55 yo
- Risk Factors
- Family history (strongest)
- Human leukocyte antigens (HLA) association
- Environmental: inorganic and organic materials (dust, mold, silica, metals, etc.)
- Classic presentations (Lofgren’s, Heerfordt) most times do not need histology for diagnosis and steroid can be started without biopsy.
- 90-95% patients have pulmonary involvement.
- Most common: Hilar lymphadenopathy
- Upon diagnosis of sarcoidosis, even without ocular symptoms, need baseline EKG and ophthalmologic exam
- Ruling out infection is critical as immunosuppression is the cornerstone for sarcoid therapy.
- Not all patients need immunosuppressive therapy!
Classic Presentations
May not need bx for confirmation
- Lofgren: arthritis (ankles, knees), erythema nodosum, bilateral hilar LN
- Heerfordt: parotiditis, uveitis, facial nerve palsy, fever, arthritis
Organ Related
Pulmonology
- 90-95% pulm involvement
- Hilar LN
- Endobronchial
- ILD
- pHTN
Ophthamology
- Anterior uveitis-most common
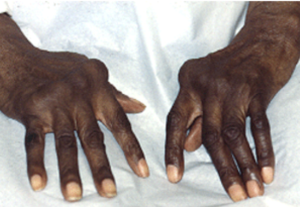
Dermatology
- EN
- Pernio
Cardiac
- Conduction abnl
- Infiltrative cardiomyopathy
Neurology
- CN palsy
- Sensorimotor polyneuropathy
- Leptomeningeal involvement
MSK
- Polyarthritis
- Osseous involvement
Lab Workup
- CBC, CMP, ESR, CRP
- Serum angiotensin- converting enzyme (ACE):
– Poor specificity and sensitivity!
– Supportive, not diagnostic - Vitamin D 25-OH, vitamin D 1,25-OH
Tests
- Baseline PFTs
- Baseline ophth exam
- Baseline EKG
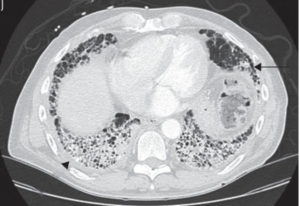
Imaging
- High res chest CT: more sens than CXR
- Suspected cardiac sarcoid: Need cardiac MRI or cardiac PET
Histology
- Shows well-circumscribed, compact, noncaseating granulomas of the epithelioid type rimmed by hyaline collagen
Infections
- Mycobacterial
- Fungal
- Mycoplasma
- PJP
- Brucellosis
- Toxoplasmosis
Environmental
- Berylliosis
- Tattoos
- Hypersensitivity pneumonitis
- Inorganic agents
Drug Induced
- TNFi
Other Autoimmune Disease
- Small-vessel vasculitis
- Inflammatory bowel disease
- Behcet’s Syndrome
- Rheumatoid nodules
Other
- Cancer
- Lymphocytic
- Interstitial pneumo
Who needs immunosuppression?
- Not all patients!
- Symptomatic (baseline or exertional)
and/or - Significant abnormalities on imaging or PFTs:
- Severe reticular disease
- Traction bronchiectasis
- Mod-sev low FVC or DLCO
Initial Therapy
- Steroids (Pred 20-30mg/d, 6mo taper
- Consider:
- Organ involved
- Disease severity
- Comorbidities
Monitoring
- Repeat ophthalmologic exams annually or with development of symptoms
- Monitor for symptoms of cardiac involvement
- Many do not ever develop symptoms and so don’t ever require therapy.
Prognosis
- After treatment, many patients have spontaneous remission
- Other patients have chronic active disease
- Lofgren syndrome prognosis good!
- 70-80% of patients in remission 2 yrs after diagnosis